Claims denials are a top revenue cycle and compliance management challenge. Preventable and unnecessary claims denials result in significant financial loss and increased compliance risk for any healthcare organization. Identifying the most common denial reasons in your organization as well as across the industry is a critical first step in preventing future denials. Medicare claims denial data is readily available from a number of sources and provides invaluable information. As an example, CGS Medicare recently published their top claims denials for April, 2020, which reflected the following data:
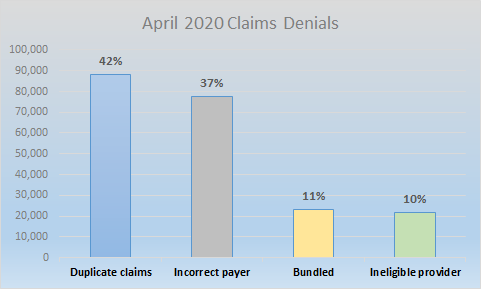
We recommend you prepare monthly reports of your claims denials. Denials, by reason, should also be trended over time to assist in identifying patterns and evaluating the effectiveness of your processes and education efforts. When evaluating your denials, things that should be considered are:
• Do you require billers to check the status of claims prior to re-submission?
• Who is responsible for adding modifiers (i.e. 50, RT, LT, 76, 77) to prevent duplicate claim denials?
• Who is responsible for obtaining demographics and verifying eligibility?
• What internal system edits are in place to identify bundled code pairs?
• Who is responsible for adding modifiers (i.e. 25, 59, XS) to prevent bundling denials?
• Who is responsible for verifying provider eligibility and enrollment?
• What are your current accuracy rates by job position?
• What education/training have you provided to prevent future denials?
• What processes should be modified to prevent future denials?
HBE’s team of certified compliance and coding experts is available to assist you with assessing your denials, implementing process improvement, preparing customized education and training and revising your policies and procedures. If you would like more information regarding our services and how we can provide valuable resources to your organization, please visit our website at www.hbeadvisors.com or email us at consulting@hbeadvisors.com

